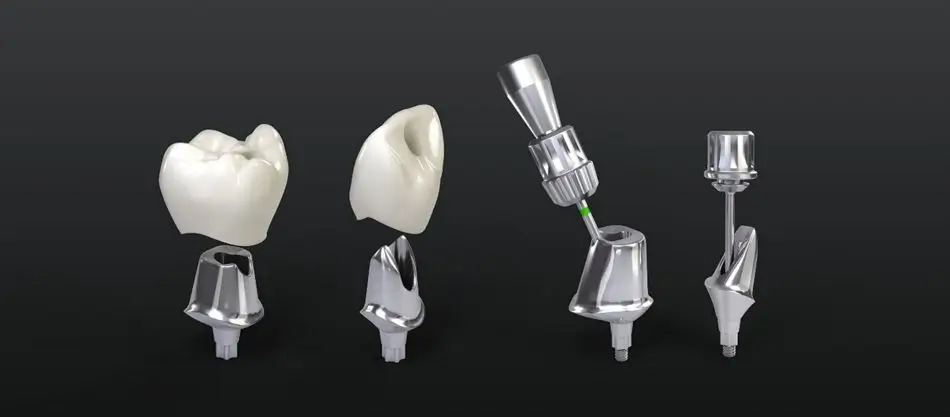
Dental implants offer a durable solution for missing teeth. Beyond the implant screw, the abutment and final prosthesis are crucial for the restoration’s success. These components connect the implant to the visible crown and significantly influence the implant’s longevity, function, and aesthetics.
The Evolution of Abutment Connections
The connection between the implant and the abutment is a critical interface that must withstand significant biomechanical forces. The stability of this connection directly impacts the success of the implant. Historically, abutment connections have been a focal point for research and development, leading to a shift from traditional designs to more sophisticated systems.
Traditional Connections: A Quick Look
For many years, the external hex connection was the industry standard. This design features a hexagonal shape protruding from the top of the implant, which mates with a corresponding recess in the abutment. While simple and widely used, the external hex is prone to certain mechanical complications, such as screw loosening and micromovement, which can lead to bacterial leakage and potential bone loss.
The internal hex connection was developed to address some of these issues. By placing the hexagonal connection inside the implant body, it provides greater stability and resistance to rotational forces. This design reduces the stress on the abutment screw and offers a better seal against bacteria.
Modern Innovations: Conical Connections
The most significant recent innovation is the widespread adoption of conical connections, also known as “cone-in-cone” or “Morse taper” designs. This type of connection features a tapered male part on the abutment that fits snugly into a matching female cone within the implant.
This design creates several key advantages:
- Cold Welding: The friction fit between the two tapered surfaces is so precise that it creates a “cold weld” or frictional lock. This virtually eliminates micromovement between the implant and abutment, providing exceptional stability.
- Reduced Screw Stress: Because the conical interface bears most of the occlusal load, there is significantly less stress on the abutment screw. This dramatically reduces the incidence of screw loosening and fracture, one of the most common complications in implant dentistry.
- Platform Switching: Many modern conical connection systems incorporate platform switching. This concept involves using an abutment with a smaller diameter than the implant platform. This shifts the implant-abutment junction inward, away from the bone, which helps preserve crestal bone levels and allows for better soft tissue volume and aesthetics.
- Superior Seal: The tight seal created by the conical connection minimizes the microgap between the implant and abutment, preventing bacterial leakage and reducing the risk of peri-implant inflammation.
Advancements in Abutment Materials
The material used to fabricate an abutment is just as important as its design. The ideal material must be strong, biocompatible, and aesthetically pleasing. While titanium has long been the gold standard, new materials are offering exciting alternatives.
Titanium: The Tried and True
Titanium and its alloys remain the most commonly used materials for abutments due to their excellent biocompatibility, high strength, and proven long-term success. They integrate well with bone and soft tissues. However, in patients with thin gum tissue, the gray color of a titanium abutment can sometimes show through, creating an aesthetic challenge, particularly in the front of the mouth.
Zirconia: The Aesthetic Champion
Zirconia has emerged as a popular alternative to titanium, especially for anterior restorations where aesthetics are paramount. This tooth-colored ceramic material offers several benefits:
- Superior Aesthetics: Its white color mimics the appearance of a natural tooth root, preventing the dark line that can sometimes appear at the gumline with metal abutments.
- Biocompatibility: Zirconia exhibits excellent soft tissue response, with some studies suggesting it accumulates less bacterial plaque than titanium.
- High Strength: While not as fracture-resistant as titanium, modern formulations of zirconia are exceptionally strong and durable enough for use in most areas of the mouth.
To combine the strength of titanium with the aesthetics of zirconia, hybrid abutments have been developed. These feature a titanium base that connects to the implant, with a zirconia structure bonded on top. This design offers the best of both worlds: the reliable, strong connection of titanium and the aesthetic appeal of zirconia where it matters most.
Innovations in Prosthetic Components
The final crown, bridge, or denture that attaches to the abutment has also seen significant innovation. The shift from traditional fabrication methods to digital workflows has transformed how prosthetic components are made.
CAD/CAM Technology
Computer-Aided Design/Computer-Aided Manufacturing (CAD/CAM) has become the standard for creating custom abutments and final prostheses. The process begins with a digital scan of the patient’s mouth and the implant position. This data is then used to design the restoration on a computer, ensuring a precise fit and ideal aesthetics. The final product is then milled from a solid block of material, such as zirconia or lithium disilicate.
This digital workflow offers greater accuracy, efficiency, and predictability compared to traditional casting methods. It also allows for the use of advanced monolithic materials that are stronger and more aesthetic than older porcelain-fused-to-metal (PFM) restorations. Making a dentist appointment in Minot, ND can provide access to professionals skilled in these modern techniques.
Screw-Retained vs. Cement-Retained Crowns
The debate between using cement or a screw to attach the crown to the abutment continues, but modern designs are making screw-retained restorations more popular. While cement-retained crowns can offer excellent aesthetics, the risk of leaving excess cement below the gumline—a major cause of peri-implantitis—is a significant concern.
Innovations in screw-retained designs, such as angled screw channels, now allow for screw-retained restorations in the anterior region without the screw access hole being visible. This provides the retrievability and soft tissue health benefits of a screw-retained crown with the aesthetics previously only achievable with cement.
Conclusion
The field of implant dentistry is constantly evolving, driven by the pursuit of better, longer-lasting, and more aesthetic outcomes for patients. The innovations in abutment connections and prosthetic components are at the forefront of this progress.